Imagine being diagnosed with a life-changing disease. Now imagine being told that because of your disease you cannot have children, before you had even thought about starting a family of your own. This is no longer the case for many patients thanks to fertility preservation. This involves procedures which help patients retain their fertility despite the effects of a disease or its treatment.
Methods of Fertility Preservation
Egg Freezing
This involves freezing unfertilised eggs. Read more…
You can also read about the limitations of egg freezing and how to maximise your chances of success here…
Embryo Freezing
This is an established technique which requires a partner”s sperm. Read more…
Ovarian Suppression
This works to reduce the damage to the ovaries during chemotherapy. Read more…
Ovarian Tissue Freezing
This is an experimental option in which doctors freeze ovarian tissue and later transplant it back into the body. Read more…
www.amitamin.com/en/fertilsan-m New life deserves the best possible start!We provide the essential building blocks for this.
Sperm Freezing
Also called sperm cryopreservation, sperm banking or semen storage. The process involves collecting and storing semen for future use. Read more…
Testicular Tissue Freezing
This is an experimental option for men which involves freezing the cells in the testicle in order to use them later. Read more…
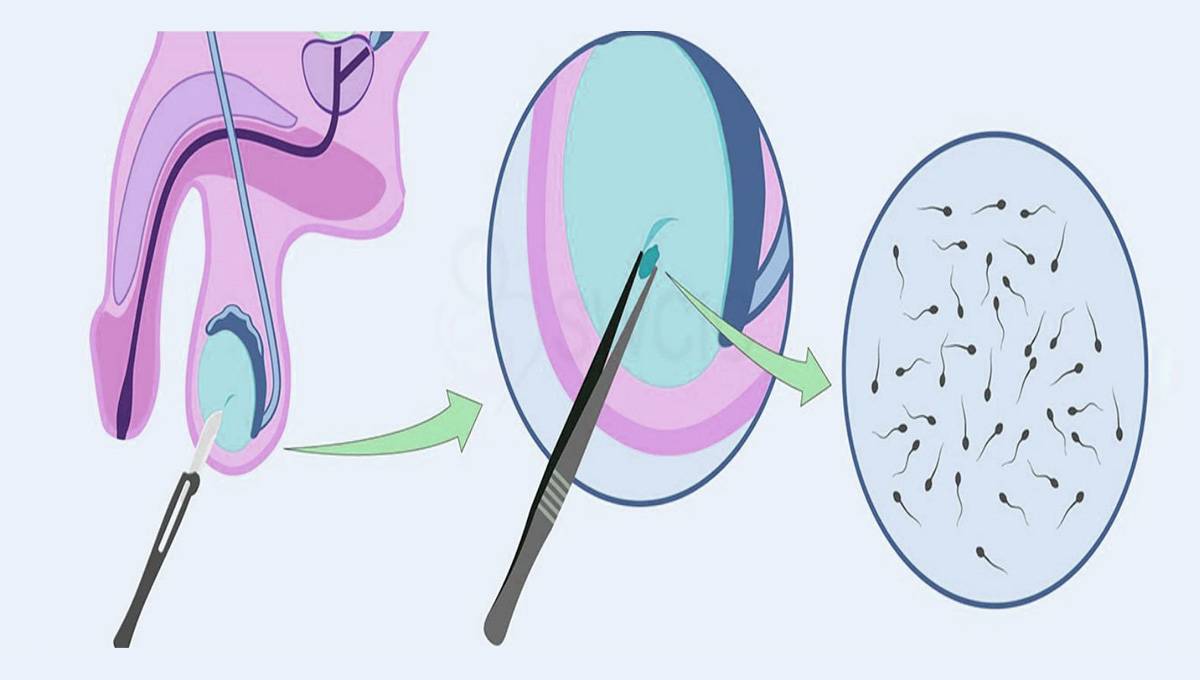
Surgical Sperm Retrieval
This is a method used to collect sperm from men who have little or no sperm in their semen. This sperm can then be used in fertility treatments. Read more…
New fertility preservation guidelines published
The British Fertility Society highlighted the importance of fertility preservation in a set of new guidelines presented at the Fertility 2018 meeting in Liverpool. These apply to people assigned female at birth. Professor Adam Balen, Chair of the British Fertility Society said “Our guidelines are designed to help our members and the wider fertility community to decide on the best course of treatment, in consultation with these patients” 1British Fertility Society. Fertility preservation: now is the moment to take action. 2018. Available from: https://britishfertilitysociety.org.uk/2018/01/04/fertility-preservation-now-is-the-moment-to-take-action/.
These guidelines are presented in a paper published in January 2018 by Ephia Yasmin from University College London Hospitals and colleagues 2Yasmin E, Balachandren N, Davies MC, Jones GL, Lane S, Mathur R, Webber L, Anderson RA. Fertility preservation for medical reasons in girls and women: British Fertility Society policy and practice guideline. Human Fertility. 2018. 21(1):3-26. Available from: https://www.tandfonline.com/doi/full/10.1080/14647273.2017.1422297. The paper addresses health conditions which may affect fertility and fertility preservation techniques.
What can affect your fertility?
Cancer
Women diagnosed with cancer may experience reduced fertility due to the cancer treatment itself. This can include chemotherapy, radiotherapy and surgery. The effect the treatment has on a woman”s fertility depends on the specific treatment. This means, for example, the exact chemotherapy drug used or the dose and site of radiation.
Unfortunately this problem faces an increasing number of women. This is because it is becoming more common to delay pregnancy until later in life, after finding a stable career. But this increases the likelihood of developing cancer before you have been able to have children.
Patient involvement is key
The guideline emphasises that the patient needs to be involved in discussions about fertility preservation as soon as possible in the treatment pathway. It is important to avoid any delay in the treatment for cancer.
Benign conditions
Besides cancer, other non-malignant diseases also affect fertility due to their treatment rather than the disease itself. These include systemic lupus erythematosus (SLE) which doctors can treat with cyclophosphamide. But this treatment can cause amenorrhoea, which is the absence of menstrual periods. Other conditions include sickle cell anaemia, aplastic anaemia and myeloproliferative diseases.
Additionally, patients undergoing pelvic surgery will likely be affected by reduced fertility. Patients may need to undergo this surgery due to endometriomas and large ovarian dermoid cysts.
Genetic and metabolic conditions
Conversely women with conditions including Turner Syndrome and galactosaemia may be at risk of reduced fertility from the disease itself, rather than the treatment. In Turner Syndrome, a young woman cannot produce her own egg cells. However she will be able to carry a baby to term. Doctors have found a potential solution to this unusual problem. Mothers of children with Turner Syndrome can donate their own eggs for freezing. Their daughter can then use these eggs when the time is right for her to start a family.
Transitioning individuals
Additionally, the study highlights the importance of counselling individuals transitioning from the female to the male gender. Freezing eggs, embryos or ovarian tissue can help people still have the choice of becoming a genetic or biological parent through pregnancy or surrogacy.
Dr James Barrett from Charing Cross Hospital said “The number of people coming forward with gender dysphoria has increased rapidly over the past decade. But the consistent provision of NHS funding for fertility preservation for this group has yet to catch up. My clinic sees around half of the patients being referred for difficulties with gender identity in the UK and although we do discuss future fertility with them, they are not always able to self-fund for the necessary procedures and ongoing storage of material. Infertility is a real disease and it is hugely frustrating that the whole NHS is not always able to help our patients with that part of their lives”.
But will these advances help the people who need them the most?
In the UK the National Institute for Health and Clinical Excellence (NICE) made promising updates to its guidelines in 2013. The changes included a recommendation that the strict criteria for NHS fertility treatment should not apply for women needing fertility preservation, and that the lower age limit should not apply.
However, in reality this is overshadowed by various constraints. These involve the power being in the hands of local Clinical Commissioning Groups (CCGs) to allocate funding. This can limit people”s access to the latest clinical developments. Furthermore if the uptake of these methods of fertility preservation increases, there will be an even greater need for a coordinated national service for the storage and access to eggs, embryos and ovarian tissue.
This is an exciting field and the latest guidelines show a huge leap towards increasing understanding of fertility preservation and the options available to patients. However more work needs to be done to be able to implement these guidelines consistently so that more patients will benefit.

Dr. Jones is an experienced consultant in assisted reproduction.
He has worked as a Fertility specialist at Kingston Hospital Assisted Conception and nearly 10 years experience of working in Obstetrics and Gynaecology across hospitals in the UK.
He completed his Masters in Assisted Reproduction Technology and then his PhD, from Imperial College London. Dr. Jones main areas of interest are Single Embryo Transfer, Endometriosis, PCOS and Implantation failure in IVF patients. He is a member of the British Fertility Society and an associate member of the Royal College of Obstetrics and Gynaecology.
Bibliography
- 1British Fertility Society. Fertility preservation: now is the moment to take action. 2018. Available from: https://britishfertilitysociety.org.uk/2018/01/04/fertility-preservation-now-is-the-moment-to-take-action/
- 2Yasmin E, Balachandren N, Davies MC, Jones GL, Lane S, Mathur R, Webber L, Anderson RA. Fertility preservation for medical reasons in girls and women: British Fertility Society policy and practice guideline. Human Fertility. 2018. 21(1):3-26. Available from: https://www.tandfonline.com/doi/full/10.1080/14647273.2017.1422297