What is embryo freezing?
Embryo freezing is also known as embryo cryopreservation. Cryopreservation is the process of freezing tissue or cells. In this case, the fertilised egg (embryo) is frozen. This preserves it until you are ready to have a child in the future, at which point the embryo can be transferred into the womb. This is a well- established technique, and it is the most effective method for fertility preservation in women.
Who would benefit from this procedure?’ link=” linktarget=” av_uid=’av-18ay6k’[/mfn]
- People with health problems which could affect their fertility in the future.
- People who are having medical treatments which could damage their fertility. This includes treatments such as chemotherapy or radiotherapy.
- People who are undergoing sex change procedures. This is because the procedures can cause partial or total infertility.
- Couples who have undergone in-vitro fertilisation (IVF) or intracytoplasmic sperm injection (ICSI) treatments. This is the most common scenario when this procedure is used. This is because IVF and ICSI can result in multiple healthy embryos which couples cannot use at the time. Therefore freezing these is a good option as a back- up or if couples decide to have another baby in the future 1 Human Fertilisation and Embryology Authority. Embryo Freezing. Internet. 2018. Available from: https://www.hfea.gov.uk/treatments/fertility-preservation/embryo-freezing/.
How does embryo freezing work?
Step 1: Egg retrieval
The first step is to stimulate egg development in a woman using hormones. After this a doctor can retrieve the egg cell, or oocyte. For this procedure the patient will be under sedation or a general anaesthetic.
Step 2: IVF
The egg cell will be fertilised by a sperm cell in a laboratory. This is called in-vitro fertilisation (IVF). Out of all the egg cells fertilised, doctors will select the best quality embryos to maximise the chances of success.
Step 3: Preparation for freezing
Embryos go through a process of development, and there are certain stages when it is best to freeze them. This can happen early on when they are just one single cell. Alternatively this can happen when it is made up of two to eight cells or in the blastocyst stage, which occurs later on. The embryologist will make this decision for you.
It is important to protect the embryos during the freezing process. When water freezes, it expands. Ice crystals can form inside the cells of the embryo which can cause damage. Therefore it is important to protect the embryo using chemicals called cryoprotectants. This replaces the water inside the cells.
Step 4: Embryo freezing
There are two methods which scientists commonly use. These are slow-rate freezing and vitrification. Vitrification uses higher concentrations of cryoprotectants and a faster cooling rate 2 British Fertility Society. Freezing and Vitrification of Gametes and Embryos. Internet. 2015. Available from: https://britishfertilitysociety.org.uk/wp/wp-content/uploads/2015/09/Freezing-and-Vitrification-of-Gametes-and-Embryos.pdf..
www.amitamin.com/en/fertilsan-m New life deserves the best possible start!We provide the essential building blocks for this.
Step 5: Storage
The next stage is to store the embryo at sub-zero temperatures in tanks of liquid nitrogen until you are ready to use them. In the UK, the standard length of time these can be stored for is 10 years, although in certain situations they can be stored for longer.
Step 6: Using the embryos when you are ready to have a child
The timing of this varies according to your individual circumstances. For people who have been newly diagnosed with a disease, they might want to delay having children until they know more about their prognosis. For people who have cancer, they might wait until they are in remission.
When you are ready, the next step is implanting the embryo. The way this will happen depends on whether you are ovulating regularly.
If you have regular periods, the doctor may suggest transferring the embryo to your womb without fertility drugs. The doctors can check that your body is ready using a number of tests. An ultrasound scan will help them check the lining of your uterus. Additionally urine or blood tests can show whether you are ovulating which is also when your body is ready to receive the embryo.
However if you have no periods or they are irregular, there are other options. The doctor can give you medicines to suppress your natural cycle and trigger a “false” period. Then the doctor can help you prepare the uterus using medications.
When your body is ready, the embryos will be thawed. Scientists will remove the cryoprotectant from the cells and replace this with water. Then the doctor will usually transfer one embryo to your womb.
What are the chances of success?
Overall this method has a high success rate and this has been increasing over the years.
Some patients are worried that the embryos will be damaged when they are frozen, and this can sometimes happen despite the scientists” best efforts to protect them. However when comparing the success rates between frozen and non-frozen (fresh) embryos, the figures are very similar.
The success rates vary according to a woman”s age. For younger women aged under 35 years old, the chances are slightly better when using fresh embryos. For women aged 35-47, the rates are the same. However for women aged over 37, the birth rate for frozen transfers is higher than fresh. Scientists think that this is because the frozen eggs were collected when the woman was younger.
Birth rate per embryo transferred using woman’s own eggs and partner sperm, 2016:
| Age range | Frozen | Fresh |
| 18-34 | 25% | 29% |
| 35-37 | 23% | 23% |
| 38-39 | 20% | 15% |
| 40-42 | 13% | 9% |
| 43-44 | 9% | 3% |
| 44+ | 4% | 2% |
Is it a good option for me?
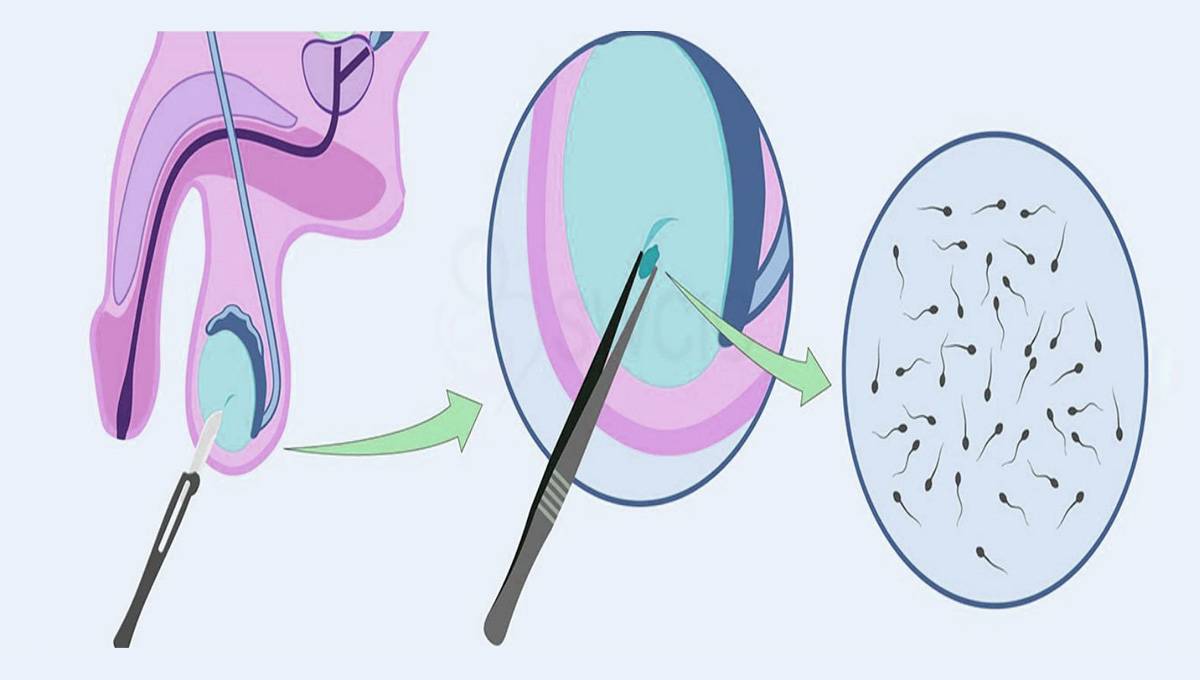
This method is tried and tested, and there are thorough protocols in place which make it a good option. However the main limitation is that you will need sperm cells, either from a partner or donor.
Additionally, it is really important to plan the timing of the procedures around other surgeries you may be having for your primary condition. For example in a woman with cancer, doctors might plan to do the egg retrieval after the excision of the tumour and before she starts chemotherapy. In this case it is important to complete the retrieval process as soon as possible to make sure that the cancer treatment is not delayed 3 Johnston KT, Potter J. Fertility Assessment and Preservation. In: Davis MP, Feyer PC, Ortner P, Zimmerman C, editors. Supportive Oncology. Philadelphia: Elsevier; 2011. p.617-623. Available from: https://www.sciencedirect.com/science/article/pii/B9781437710151000588.
Timing might be particularly problematic if the disease is very severe and you need urgent treatment. In this scenario there might not be enough time to undergo the first step of hormone stimulation to encourage egg development.
The most important thing to bear in mind is that your options will depend on your individual situation. You should discuss these with your doctor to form a tailored approach to your treatment. This will help you to have a child in the way that is best for you, whilst maximising your health and wellbeing.

Dr. Jones is an experienced consultant in assisted reproduction.
He has worked as a Fertility specialist at Kingston Hospital Assisted Conception and nearly 10 years experience of working in Obstetrics and Gynaecology across hospitals in the UK.
He completed his Masters in Assisted Reproduction Technology and then his PhD, from Imperial College London. Dr. Jones main areas of interest are Single Embryo Transfer, Endometriosis, PCOS and Implantation failure in IVF patients. He is a member of the British Fertility Society and an associate member of the Royal College of Obstetrics and Gynaecology.
Bibliography
- 1Human Fertilisation and Embryology Authority. Embryo Freezing. Internet. 2018. Available from: https://www.hfea.gov.uk/treatments/fertility-preservation/embryo-freezing/
- 2British Fertility Society. Freezing and Vitrification of Gametes and Embryos. Internet. 2015. Available from: https://britishfertilitysociety.org.uk/wp/wp-content/uploads/2015/09/Freezing-and-Vitrification-of-Gametes-and-Embryos.pdf.
- 3Johnston KT, Potter J. Fertility Assessment and Preservation. In: Davis MP, Feyer PC, Ortner P, Zimmerman C, editors. Supportive Oncology. Philadelphia: Elsevier; 2011. p.617-623. Available from: https://www.sciencedirect.com/science/article/pii/B9781437710151000588